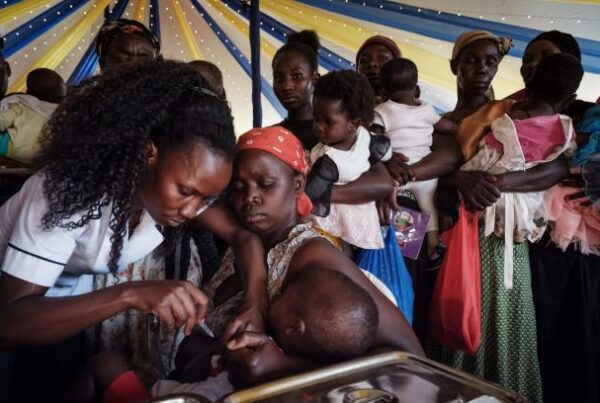
BY VICTORIA AMUNGA | 5484 MEDIA | KENYA
STORY HIGHLIGHTS
- Exclusive breastfeeding remains at around 60%, below Kenya’s 80% target
- Breastfeeding Mothers Bill advances in Parliament, but not yet enacted
- Workplace gaps cited as major barrier, echoing global challenges from the US to South Africa
Kenya is attempting to reinvigorate efforts to improve breastfeeding protections and support for working mothers, as exclusive breastfeeding rates remain largely unchanged at around 60%.
The renewed push centres on the proposed Breastfeeding Mothers Bill, 2024, which seeks to strengthen workplace protections and mandate lactation spaces across both public and private sectors.
While advocates say legislative momentum has picked up since 2024, the Bill has yet to be enacted into law, raising concerns among maternal health experts about implementation delays.
Globally, breastfeeding policy has become a central pillar of child nutrition strategies, with governments from Brazil to Norway investing heavily in workplace reforms and community health campaigns to raise exclusive breastfeeding rates.
Bill Advances but Awaits Enactment
The Breastfeeding Mothers Bill was tabled in Parliament by MP Sabina Chege and passed its first reading in May 2024. It advanced to public participation by August the same year, proposing:
- Mandatory lactation rooms in workplaces
- Paid breastfeeding breaks
- Stronger enforcement mechanisms
- Protection from workplace discrimination
By late 2025, lawmakers signalled intent to fast-track the Bill during discussions at a Reproductive, Maternal, Newborn, Child and Adolescent Health (RMNCAH+) forum, alongside other health legislation.

However, as of early 2026, the Bill has not been formally enacted.
Parliamentary reviews in early 2025 examined its provisions, but implementation remains pending — a pattern that health advocates say reflects a broader gap between legislative ambition and execution.
Similar legislative delays have been seen in other countries. In the United States, for example, workplace lactation protections expanded only recently under federal labour reforms, while several African nations have struggled with enforcement despite having policy frameworks in place.
Policy Exists — But Implementation Lags
Kenya already has provisions under the 2017 Health Act that require employers to provide lactation spaces and breastfeeding breaks.
In addition, the 2020–2024 Breastfeeding-Friendly Workplace Implementation Framework was designed to guide employers in operationalising these requirements.
Yet enforcement has been uneven.
In October 2025, the Ministry of Health reiterated its call for employers to comply with the guidelines, citing gaps in both infrastructure and monitoring.
Health officials say workplace constraints, cultural norms and limited community support contribute to stagnation in exclusive breastfeeding rates, which dipped slightly from 61% to around 60% in 2025.
Kenya’s national target stands at 80%.
By comparison, Rwanda and Sri Lanka have reported higher rates following sustained community-level interventions, while the United Kingdom continues to face low exclusive breastfeeding rates at six months despite advanced health systems.

Community and Health System Interventions
Beyond legislation, Kenyan health authorities and research institutions have emphasised strengthening frontline health worker training in line with World Health Organization recommendations.
Initiatives include:
- Expansion of the Baby-Friendly Community Initiative (BFCI)
- Adaptations of the Baby-Friendly Hospital Initiative (BFHI)
- Enhanced data systems to track nutrition outcomes
- Increased community engagement through maternal health forums
The African Population and Health Research Center (APHRC) has highlighted the importance of integrating legal reform with public awareness campaigns and monitoring systems.
A parliamentary forum in 2025 generated commitments to improve nutrition data collection and enforcement mechanisms, although measurable shifts in breastfeeding rates have yet to materialise.
Why It Matters — At Home and Abroad
Breastfeeding is widely recognised by the World Health Organization as a cost-effective intervention to reduce infant mortality, improve cognitive development and lower long-term health risks.
For Kenya — and for the wider African diaspora community — the issue extends beyond maternal rights to long-term public health and economic productivity.
Health economists note that improving breastfeeding rates can significantly reduce healthcare costs associated with preventable childhood illnesses.
As lawmakers debate the next steps, observers say the challenge is no longer policy design, but enforcement — ensuring that protections move from paper to practice.
Whether Kenya can close that implementation gap may determine if it meets its 80% target — and whether its legislative push becomes a model for other middle-income countries balancing workforce participation and maternal health protections.