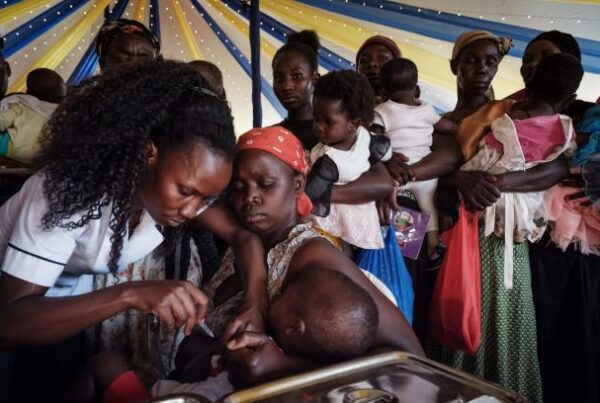
A child receives a shot during the launch of the extension of the worlds first malaria vaccine (RTS, S) pilot program for children at risk of malaria illness and death within Kenyas lake-endemic region at Kimogoi Dispensary in Gisambai on March 7, 2023. – The pilot program coordinated by the World Health Organization (WHO) has provided malaria vaccines in three countries, Ghana, Malawi and Kenya, since 2019. More than 1.2 million children under five years old have received at least one dose of the four-dose vaccine in Africa. According to the WHO, the vaccine has been estimated to save one childs life for every 200 children vaccinated. Around 90 percent of the world’s malaria cases are recorded in Africa, where 260,000 children die from the disease each year. (Photo by YASUYOSHI CHIBA / AFP) (Photo by YASUYOSHI CHIBA/AFP via Getty Images)
BY NAOMI WANDIA | 5484 MEDIA | KENYA
STORY HIGHLIGHTS
- Nationwide insurance for 107,000 Community Health Promoters from July 2026 to strengthen grassroots maternal care
- Maternal mortality remains more than double the global average, despite recent declines
- Kenya’s reforms mirror broader African efforts to scale community-led healthcare and reduce preventable deaths
Kenya has announced a major expansion of insurance coverage for more than 107,000 Community Health Promoters (CHPs) as part of an intensified national effort to reduce maternal deaths and strengthen universal health coverage, amid growing global concern over preventable maternal mortality.
Health Cabinet Secretary Aden Duale said the initiative aims to protect frontline health workers while improving early detection of pregnancy complications at the household level — a strategy increasingly viewed by global health experts as critical in countries with stretched hospital systems.
Kenya’s maternal mortality ratio is estimated at about 530 deaths per 100,000 live births, down from previous years but still significantly higher than the global average of roughly 197 per 100,000. Across sub-Saharan Africa, the region accounts for nearly 70% of global maternal deaths, according to UN and WHO estimates.
The government’s latest measures form part of wider reforms under the country’s Universal Health Coverage (UHC) agenda, including investments in primary facilities such as Riruta Health Centre to equip them with theatres capable of handling emergency obstetric complications like postpartum haemorrhage and pre-eclampsia — two leading causes of maternal deaths across Africa.
Health experts estimate that improved access to timely emergency obstetric care could help prevent thousands of maternal deaths annually in Kenya, where roughly 6,000 women are still estimated to die each year from pregnancy-related complications.
Insurance Cover for Community Health Promoters
From 1 July 2026, all 107,000 CHPs will receive comprehensive insurance cover funded jointly by national and county governments under a 50:50 cost-sharing model.
The cover is expected to include primary healthcare services, laboratory tests and treatment support, recognising CHPs as essential workers who serve as the first point of contact in rural and informal settlements.
Kenya’s community health workforce plays a crucial role in:
- Identifying high-risk pregnancies
- Promoting antenatal care attendance
- Supporting immunisation and nutrition programmes
- Educating families on safe delivery and newborn care
The initiative builds on years of training support from organisations such as Amref Health Africa and other public health partners, which have helped professionalise Kenya’s community health model.
Officials say improved stipends, insurance and structured supervision will allow CHPs to reach vulnerable households more consistently, particularly in arid, remote and low-income urban areas where hospital access remains limited.
Accountability and Public Trust After Hospital Death Probe
The reforms come amid heightened scrutiny of maternal care following the death of Grace Wambui Misigo at St. Elizabeth Mukumu Mission Hospital in Kakamega County in February.
A Ministry of Health investigation is examining allegations of negligence after an autopsy reportedly linked the death to ruptured internal organs.
In response, the government has introduced a new national toll-free hotline to report maternal and neonatal care concerns, part of a broader accountability drive aimed at rebuilding public trust in the health system.
Kakamega County has already rolled out anti-shock garments, newborn care units and emergency response strategies under its “zero maternal and neonatal deaths” campaign.
Diaspora Impact and Global Relevance
For Kenya’s diaspora — whose remittances exceeded KSh 649.7 billion (about $5 billion) in 2025 — maternal healthcare remains a major area of financial support for families back home.
Studies show that remittance-supported households are more likely to access skilled birth attendants, antenatal clinics and emergency referrals, directly influencing maternal and child survival outcomes.
With more than 29 million Kenyans now enrolled under the Social Health Authority framework, the government says the reforms could significantly ease the financial burden on families who often rely on overseas relatives to cover medical expenses.
Africa-Wide Parallel: Community Health as a Lifeline
Kenya’s strategy reflects a broader continental shift toward community-led maternal healthcare.
- In Ethiopia, the Health Extension Worker programme has significantly improved antenatal care coverage in rural regions.
- Rwanda’s community health insurance model has helped drive one of Africa’s fastest declines in maternal mortality over the past two decades.
- Ghana’s Community-based Health Planning and Services (CHPS) system has expanded skilled birth attendance in underserved communities.
Similarly, Nigeria — Africa’s most populous nation — has scaled up community midwifery schemes to address high maternal mortality rates, particularly in northern regions where access to hospitals remains limited.
Public health analysts say these models demonstrate that strengthening frontline health workers is one of the most cost-effective ways to reduce maternal deaths across low- and middle-income countries.
A Long-Term Vision for Health Sovereignty
The maternal health push also aligns with President William Ruto’s broader health sovereignty agenda, which includes ambitions to manufacture 60% of vaccines locally by 2040 and reduce reliance on external medical supply chains.
Globally, the UN Sustainable Development Goals target a maternal mortality ratio below 70 deaths per 100,000 live births by 2030 — a benchmark many African nations, including Kenya, are racing to meet.
If effectively implemented, Kenya’s insurance-backed community health model could offer a scalable blueprint for other African countries and diaspora-supported health systems seeking to reduce preventable maternal deaths while expanding universal healthcare access.